PawVerde.com – pet allergies represent a complex immune response to proteins found in animal dander, saliva, and fur, affecting millions of pet owners and their animals worldwide. These allergic reactions manifest through diverse symptoms in both humans and pets, ranging from respiratory distress and skin irritation to behavioral changes. Accurate identification and early diagnosis of these symptoms are essential for effective management and treatment, preventing progression to severe conditions such as asthma or chronic skin infections.
In pets, allergic reactions primarily result from hypersensitivity to environmental allergens such as pet dander, pollen, dust mites, and certain foods. Humans commonly develop allergic responses upon exposure to proteins found in pet saliva and dander, which can exacerbate respiratory and dermatological symptoms. This article explores the signs of pet allergies in both pets and humans, diagnostic methodologies, treatment strategies, and emerging research insights relevant to allergists, veterinarians, and pet owners.
Recognizing Signs of Pet Allergies in Pets
Allergic manifestations in pets, particularly dogs and cats, often present as a combination of behavioral and physical symptoms. Behavioral indicators include excessive scratching, persistent licking, and chewing focused on specific body areas, often corresponding to sites of inflammation or irritation. Such behaviors are not merely discomfort responses but reflect underlying immune-mediated skin hypersensitivity.
Physical signs in allergic pets typically involve erythema (skin redness), papular rashes, hair loss (alopecia), and recurrent ear infections (otitis externa). These dermatological symptoms frequently affect the face, paws, abdomen, and ears. The presence of chronic otitis in pets is strongly associated with allergic dermatitis, often complicating diagnosis due to overlapping infectious etiologies. Additionally, gastrointestinal symptoms such as vomiting and diarrhea may indicate food allergies, a less common but significant subset of pet allergies requiring elimination diet trials for confirmation.
Differences in allergy presentations between dogs and cats are notable. Dogs frequently exhibit generalized pruritus and secondary bacterial or yeast infections, while cats may display miliary dermatitis, self-induced alopecia, and eosinophilic granuloma complex. Seasonal exacerbations correspond with increased environmental allergen exposure, such as pollen or mold spores, necessitating temporal considerations in symptom evaluation.
Identifying Pet Allergy Symptoms in Humans
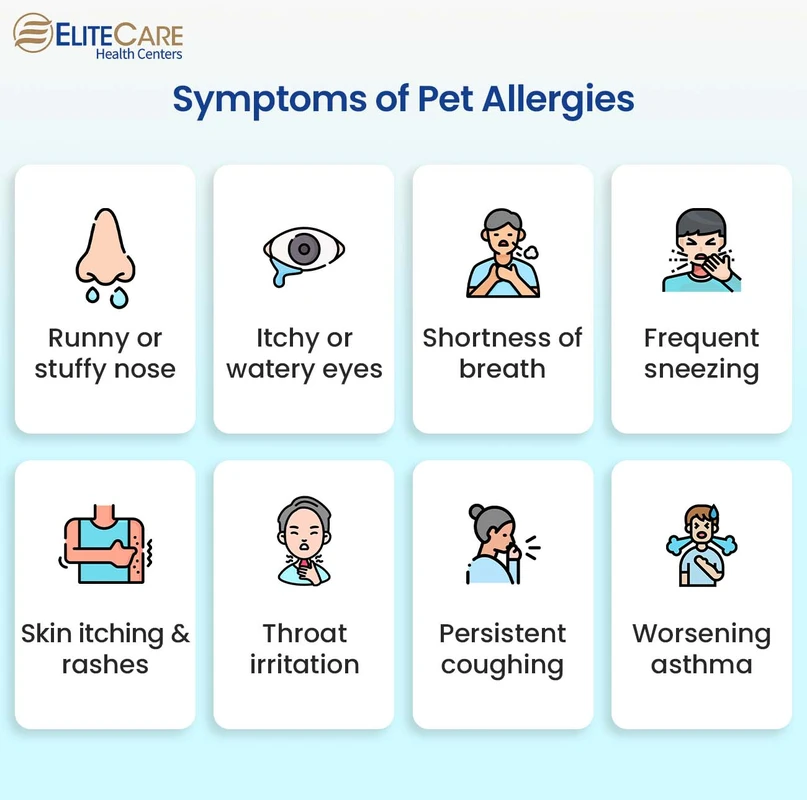
In humans, pet allergies predominantly manifest through respiratory and dermatological symptoms triggered by exposure to pet dander and saliva proteins. Respiratory symptoms include sneezing, nasal congestion, runny nose (rhinorrhea), and wheezing, with some individuals progressing to allergic asthma characterized by bronchial hyperresponsiveness and inflammation.
Ocular symptoms present as itchy, red, and watery eyes (allergic conjunctivitis), often accompanying nasal symptoms. Cutaneous reactions range from localized urticaria (hives) to generalized eczema-like rashes following skin contact with pets. Notably, children and individuals with pre-existing atopic conditions, such as asthma or eczema, exhibit increased susceptibility to severe allergic responses.
The impact of pet allergies on pediatric populations carries significant clinical implications. Studies indicate that early-life exposure to pet allergens can modulate immune system development, with conflicting evidence regarding protection versus sensitization. Nonetheless, children with established pet allergies require vigilant monitoring to mitigate exacerbations of asthma and other respiratory conditions.
Diagnostic Methods for Pet Allergies
Accurate diagnosis of pet allergies involves a combination of detailed medical history, physical examination, and confirmatory allergy testing. A comprehensive clinical history should document symptom patterns, timing relative to pet exposure, and environmental factors, facilitating differential diagnosis from other allergic or infectious diseases.
The skin prick test remains the gold standard in allergy diagnostics. This minimally invasive procedure introduces small amounts of standardized allergen extracts into the epidermis, eliciting a wheal-and-flare reaction in sensitized individuals within 15-20 minutes. Interpretation requires expertise to distinguish true positives from irritant or false-positive responses, especially in patients with dermatographism or skin conditions.
For patients unable to undergo skin testing, blood assays measuring allergen-specific Immunoglobulin E (IgE) provide an alternative. These tests quantify circulating IgE antibodies directed against pet allergens, offering objective data to support clinical findings. However, blood tests generally exhibit lower sensitivity compared to skin prick testing.
In veterinary medicine, allergy diagnosis incorporates intradermal skin testing analogous to human protocols, supplemented by elimination diet trials to identify food allergens. These trials involve feeding pets hypoallergenic diets for 8-12 weeks, monitoring symptom resolution, and subsequently reintroducing suspected allergens to confirm causality.
Managing and Treating Pet Allergies
Effective management of pet allergies requires a multifaceted approach combining environmental control, pharmacotherapy, and immunomodulation. Environmental interventions include regular cleaning to reduce allergen load, use of high-efficiency particulate air (HEPA) filters, and maintaining pet hygiene through consistent grooming to minimize dander dissemination.
Pharmacological treatments in humans typically involve antihistamines to alleviate sneezing and itching, intranasal corticosteroids to reduce nasal inflammation, and leukotriene receptor antagonists for asthma control. In severe or persistent cases, allergen-specific immunotherapy (AIT) offers disease-modifying potential by desensitizing the immune system through controlled allergen exposure, with evidence supporting long-term symptom reduction.
For pets, veterinarians prescribe topical treatments such as medicated shampoos and corticosteroids to manage skin inflammation. Systemic therapies include antihistamines and in refractory cases, immunotherapy tailored to identified allergens. Food allergy management emphasizes strict adherence to elimination diets to prevent recurrent gastrointestinal and dermatological symptoms.
Prompt veterinary or medical consultation is recommended for individuals exhibiting progressive symptoms, respiratory distress, or secondary infections. Preventive strategies for pet owners encompass allergen avoidance, strategic pet selection, and educating families on early symptom recognition.
Emerging Research and Considerations

Recent studies highlight the immunological complexity differentiating dog and cat allergies, with cat allergens (notably Fel d 1) demonstrating higher airborne persistence and sensitization potency compared to canine allergens. This disparity influences exposure risk assessments and therapeutic targeting.
Parental preconception and early childhood exposure to pets remain under investigation regarding their roles in allergy development. Some longitudinal cohort analyses suggest that controlled exposure may induce immunological tolerance, while others report increased sensitization, underscoring the need for personalized risk evaluation.
Misconceptions persist regarding pet allergies, including the belief that certain breeds are hypoallergenic. Scientific consensus refutes this, emphasizing that allergen production varies minimally across breeds, and exposure reduction strategies remain paramount.
Ongoing research focuses on novel diagnostic biomarkers and immunotherapeutic modalities, including recombinant allergen vaccines and monoclonal antibodies targeting IgE pathways, promising enhanced precision in allergy management.
FAQ
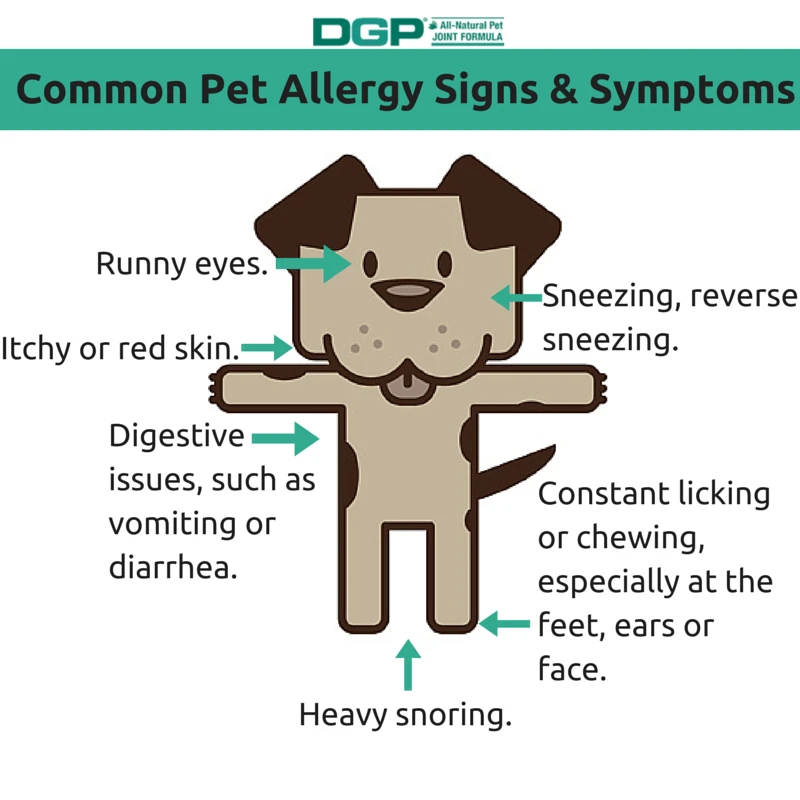
What are the earliest signs of pet allergies in dogs and cats?
Early signs in dogs and cats include persistent scratching, licking, and chewing, especially around the face, paws, and ears, accompanied by redness, hair loss, and occasional ear infections. These behavioral and physical changes indicate underlying allergic inflammation.
How do doctors diagnose pet allergies in humans?
Physicians use skin prick testing as the primary diagnostic tool, introducing small amounts of pet allergens into the skin to observe reactions. Blood IgE tests serve as supplementary diagnostics, especially when skin testing is contraindicated.
Can pet allergies cause asthma?
Yes, exposure to pet allergens can trigger asthma symptoms, including wheezing and difficulty breathing, particularly in sensitized individuals or those with pre-existing respiratory conditions.
Are there effective treatments to reduce pet allergy symptoms?
Treatment options include antihistamines, corticosteroids, and allergen immunotherapy for humans, alongside environmental modifications. Pets benefit from veterinary-prescribed topical and systemic therapies and allergen avoidance strategies.
Is it true that some dog or cat breeds do not cause allergies?
No breed is completely hypoallergenic. All cats and dogs produce allergens; however, individual allergen levels may vary slightly. Managing exposure remains the most effective approach to control symptoms.
Pet allergies require vigilant recognition and tailored management to mitigate health impacts on both pets and their owners. Advances in diagnostic precision and immunotherapy promise improved outcomes, while ongoing research continues to refine understanding of allergen biology and immune responses. Pet owners are encouraged to collaborate closely with veterinary and medical professionals to develop comprehensive allergy control plans that accommodate individual sensitivities and environmental factors.